According to the CDC, 18.6 million Americans develop knee pain each year, and 4 million develop hip pain. Joint pain is one of the most common problems Americans face today. Until we figure out how to rejuvenate damaged joints, you’re born with one pair of hips, knees, ankles, and shoulders for life — so doing what we can to preserve them matters.
Risk factors for joint pain
There are risk factors that increase the rate of joint damage and pain. Age is perhaps the most influential. Over time, wear and tear inevitably accumulate and cause pain, stiffness, and inflammation.
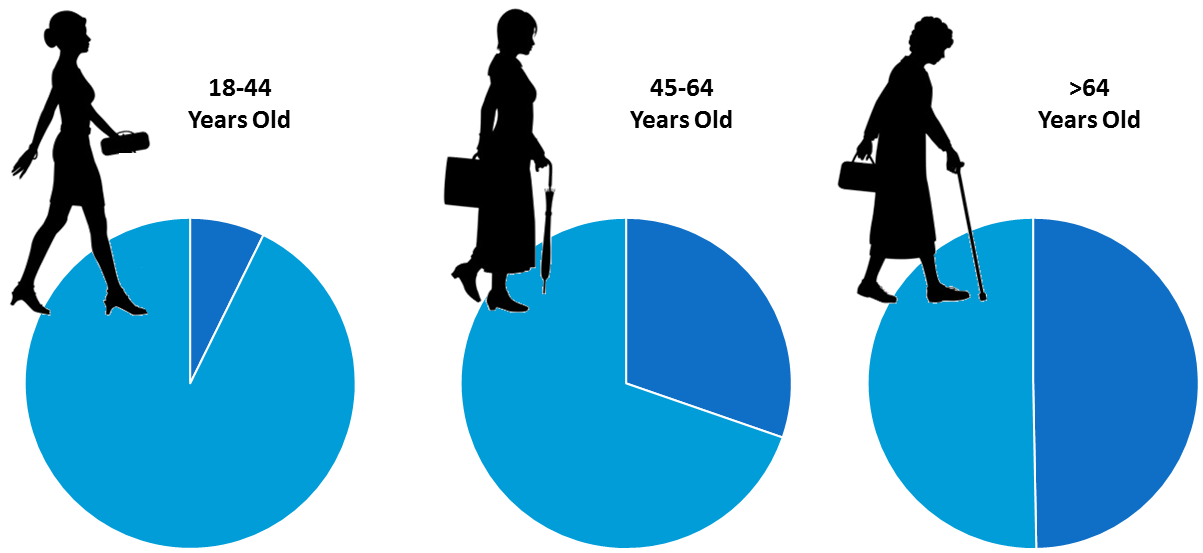
An estimated 62% of adults with arthritis are under 65. Specifically:
- Ages 18 – 44: 7.3% ever reported doctor-diagnosed knee arthritis
- Ages 45 – 64: 30.3% ever reported doctor-diagnosed knee arthritis
- Ages 65+: 49.7% ever reported doctor-diagnosed knee arthritis
Nothing stops the march of time. But there are modifiable risk factors that we can influence:
- Work-related factors — frequent heavy lifting, kneeling, stair climbing, and prolonged standing. A jack-hammer operator has more wear and tear than a desk worker. If pain becomes debilitating and your job is high-demand, a longer-term solution that involves a less joint-stressful occupation is worth considering.
- Activity-related factors — your recreational sports may also be contributing. Marathon running, for example, is high-impact on the knees. For some patients, the “runner’s high” is worth the incremental damage — that’s an individual lifestyle decision. Cross-training with lower-impact alternatives is usually the right compromise.
- Weight-related factors — probably the most important modifiable risk factor. Two in three obese Americans will develop symptomatic knee OA in their lifetime. While walking down stairs, the knee experiences forces up to 9 times body weight.
So what can you do? Five strategies, in the order I prioritize them in clinic.
Maintain flexibility and joint mobility.
Limited joint motion forces the muscles to stop acting as shock absorbers.
Maintaining joint mobility and range of motion is key to optimizing joint function. When joint motion is limited, it places additional stress on the joint itself.
Greater excursion of a joint facilitates greater transmission and dissipation of forces by the surrounding muscles, rather than at the joint surface. Muscles around a joint act like dampening mechanisms — they decelerate motion across the joint. If joint motion is limited, the surrounding muscles can’t serve as dampers. So flexibility work isn’t about touching your toes; it’s about letting your muscles do their job of protecting the joint.
Lose weight, even a little.
A 10-lb weight loss feels like 40 lb less across the knees. Patients report ~20% pain reduction per 10 lb.

During the gait cycle there are several points where your entire body weight is propelled off of one leg. With each step you take, two to four times your body weight is transmitted through the knee joint.
Due to the physics of locomotion, even a weight loss as small as 10 lbs can translate to your knees feeling as much as 40 lbs lighter. Studies show that people with arthritic knees lose about 20% of their pain with every 10 pounds of weight loss. For some patients, that can be the difference between surgery and no surgery.
“Imagine walking around all day with a backpack that had a 10-pound weight in it. You would quickly feel how achy your back, hips and knees were towards the end of the day.”
Many people fail to recognize the role weight plays in joint function. Even though your weight may double over time, your joints and bones do not increase proportionately to support the additional load. After skeletal maturity (mid-20s), bone mass has peaked, and a slow irreversible decline begins. Any additional weight concentrates greater forces on a skeleton built to support your ideal body weight.
Choose joint-sparing exercise.
Cartilage is nourished by movement. Disuse weakens supporting muscles and accelerates deterioration.
This is the most common question I field in clinic. Many people avoid exercise as joint pain progresses — but that actually promotes more rapid joint deterioration, stiffening, and pain. Cartilage, the substance that lines joint surfaces and facilitates smooth movement, is nourished by joint motion. Disuse of any joint leads to progressive weakening of the muscles around it.
Not all exercises are created equal. Once joint pain sets in, choose exercises that preferentially spare the affected joint but still promote motion. Lowest-impact options first:
- Swimming and aquatic exercise — near-zero joint loading. The single best exercise for an arthritic knee.
- Cycling — non-weight-bearing, builds quadriceps without impact.
- Elliptical — low impact, full range of motion.
- Walking — about 1× body weight on each step; well tolerated by most knees.
- Stair climbing — significantly more joint load; tolerate only if pain allows.
- Running — high impact (3 – 4× body weight per step). Best minimized once OA is established.
Aquatic exercises are excellent choices if land-based ones aggravate the knees or other joints. Information about local arthritis-friendly programs is available at arthritis.org.
Maintain good posture.
Off-center alignment makes muscles work overtime and dump force back onto the joints.
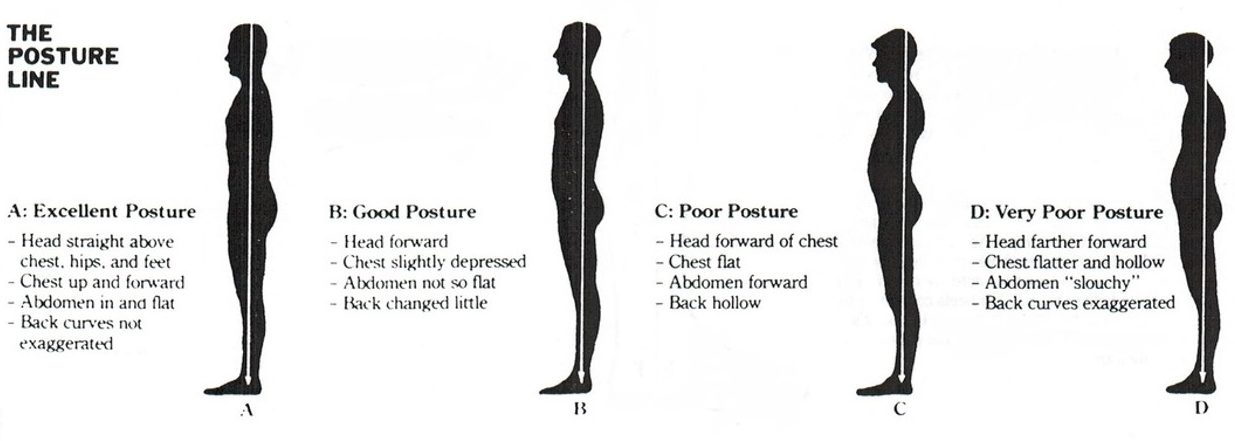
Posture is about placing your body in the optimal position for joints to function. The more your body is off-center, the harder your muscles have to work to maintain position. Those muscles eventually fatigue and dump strain back onto the joints.
Maintaining good posture takes advantage of how your joints were designed to work. You want your head centered over your shoulders, ears aligned with your shoulders, and your torso centered over your pelvis. A strong core (abdomen and lower back) promotes good posture and ultimately lessens the pressure on your hips, knees, and ankles.
Planks, back extensions, yoga, and Pilates all help strengthen the core musculature that holds you upright.
Strengthen the muscles around the joint.
Stronger muscles absorb shock that would otherwise hit the joint. No pain, no ‘gain’ — pain isn’t the goal.
Muscle strengthening helps sore joints. Muscles support a joint and absorb shock and force. Stronger muscles around a joint reduce the force experienced at the joint itself, which alleviates pain and discomfort.
For the lower extremities, stretching and strengthening the hamstrings, hip flexors, and quadriceps (particularly the often-neglected vastus medialis oblique) at least three times a week can help.
When developing a strengthening program, choose an exercise routine you enjoy that doesn’t hurt. While muscle achiness and soreness can be acceptable in healthy training, when you have arthritis there’s no gain in pain. A good rule of thumb: monitor how long pain or achiness lasts after a workout. If you still have significant pain and swelling 24 hours later, re-evaluate the exercises you’re doing. A trainer or physical therapist can help.
If joint pain has slowed you down, call 281-690-4678 or request a consultation so we can build a strategy together. Many patients get years more out of their knees and hips with a thoughtful non-operative plan — and when surgery does become the right move, you arrive at it stronger and more prepared.
Sources